Experience Living with PCOS

The first time I had symptoms of PCOS was as an adolescent when I think back on it. Without getting to graphic, I will instead allow this to be the start of many hubs posting my personal journey as well as my findings pertaining to medications, support groups, cures, and the latest news from health professionals. Since I am a Christian individual, I have faith that we can be healed of any ailment, on one level or another. I also know that God uses some doctors to do great works with medications and science.
With Polycystic Ovarian Syndrome as a young female I did not know what my body was telling me. My mother would ask the doctor detailed questions about my variations of menses. Now that I have been diagnosed, I have gain knowledge in this. My doctor never thought to run an extensive panel of hormonal blood testing’s. When I was having those symptoms even as a adolescent my hormones were trying to tell me something was not right when I was at the age of around 12. At age ten I began my menses and was perfectly normal at that time. It was only after two years had passed I began going months without one and going some two to three weeks with it. It was very confusing for a young female to experience. As I grew older this had began what I called “my normal”. Throughout my teenage years I would experience sharp-to-dull pain and a weird feeling much like a ripple in water in my lower abdominal area, more noticeably in my pelvic region were the ovaries are located. The pains were becoming more frequent over the years and I made my doctor aware of my pains and concerns. This did not lead to anything but wrong information, I was told there was nothing wrong with me from being told that there were outrageous health issues going on with me.
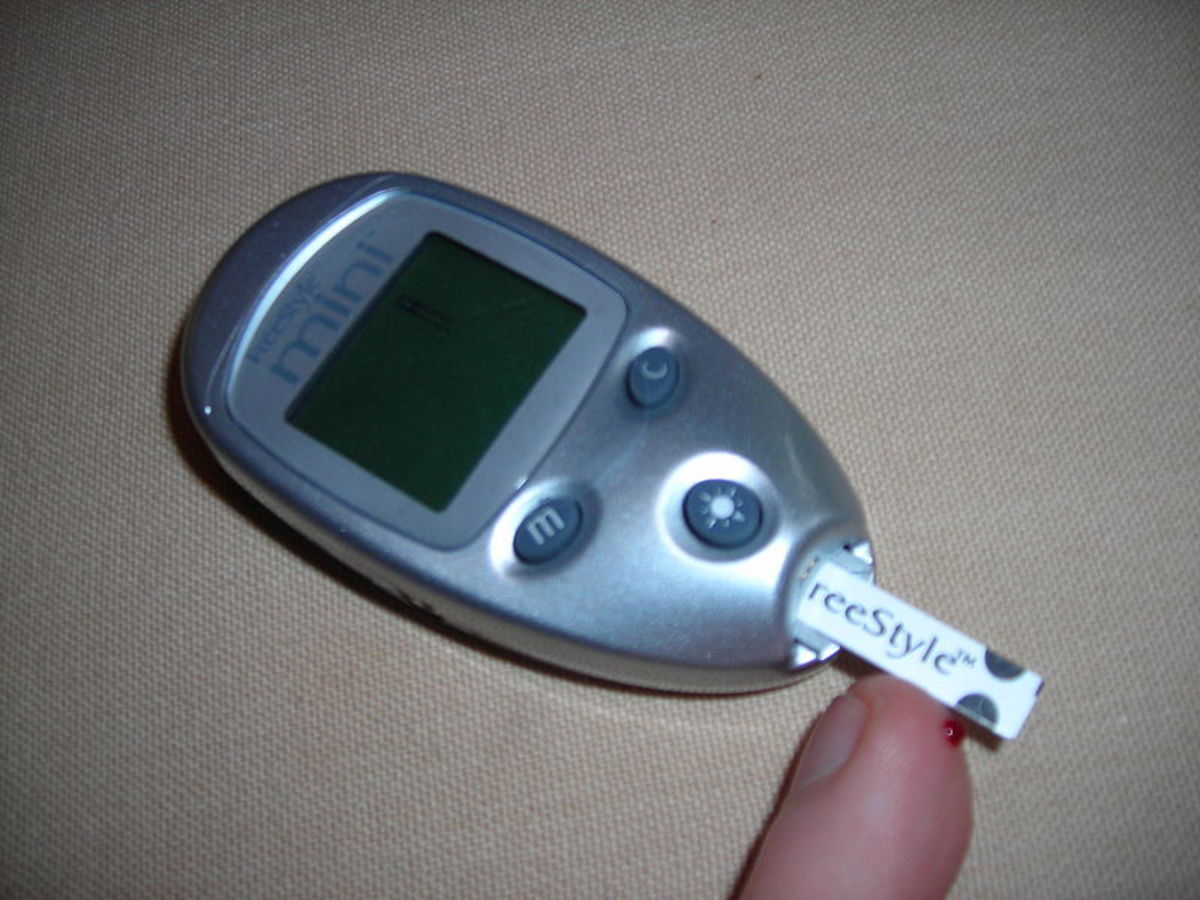
There came a time where I did find a doctor around age thirty at a well-known hospital in my city. I was thankful for her findings and her explanations, and goals that she set out for me. Upon finding my tumor-on my right ovary, also known as a cyst, my doctor at that time still did not make the connection between me complaining of nausea, dizziness, and slight sweatiness with me having diabetes. If you were not aware of PCOS, I’m sure you are not aware of how diabetes plays a part in having PCOS. Pre and Type 2 Diabetes is closely link with PCOS and is often one sign a person experience when having this syndrome. As reported by Insulite Labortories, “Certain factors that figure in the onset of PCOS are also implicated in the development of Pre- and Type 2 Diabetes: excessive abdominal fat, high LDL "bad" blood cholesterol and low HDL "good" cholesterol, high levels of triglycerides and hypertension (high blood pressure).”
The ovaries are part of the endocrine system, which regulates the body's hormones, including the hormones that govern menstruation as well as production of insulin -- another hormone critical to metabolism. Dr. Geoffrey Redmond, an endocrinologist specializing in women's health, said there is no question about the association. He goes on to report that PCOS appears to be genetic, particularly among women with family histories of diabetes. Although dietary restrictions, such as cutting down on carbohydrates, and exercise can influence the body's hormone levels and even improve insulin sensitivity, PCOS is not curable. However, with a magnesium supplement, complementary & alternative therapies, contraceptives or other hormone-based medications this disorder can be managed or cured.
There are two directions a person may explore with faith of being cured, Western Medications or Contemporary & Alternative Therapies. Both have been proven to work on a vast amount of women. With this in mind exploring both sides are worth researching. Western medications consist of a fixed-variable schedule of medications such as Metformin (Glucophage), birth control pills, testosterone, Clomid, or gonadotropins (LH-releasing hormone-LHRH). These medications range in side effects, severity or fertility issues and urgency, and personal or biological tolerance.
I urge every female to not only to pay attention to what her body is telling her but to take an active approach and alarm your gynecologist and/or medical physician of your symptoms, changes, or findings.